What is eczema?
Eczema is a condition that can cause your skin to turn red, scaly and itchy. It is often referred to simply as atopic dermatitis or atopic eczema. If you have eczema, you may also have blisters or an inflamed skin rash. It is more common with infants, but most infants outgrow it by around the age of 10. About 3% of adults and children suffer from this skin condition.
There is no cure for eczema, but it does come and go. In fact, you may have long stretches of time without any flare-ups. There are products available to help effectively manage and ease the symptoms of eczema.
It is unknown exactly what causes eczema, but there are factors that can trigger flare-ups, which we’ll get to in a bit. Additionally, eczema is more common in people who have a familial history of allergies or asthma.
One of the most distressing symptoms of atopic dermatitis is the itchiness. If you scratch or rub a patch of skin with eczema, you can actually make it worse and even more itchy.
What does eczema look like?
There are a number of different types of eczema, but we’ll focus on Atopic Dermatitis and Contact Dermatitis for this article. Common symptoms for all types of eczema are:
- redness
- itching
- scaly, dry skin
Depending the type, location and severity of the eczema, it may present itself in a variety of ways. Here are a couple of examples:

What causes eczema flare ups on the face?
Atopic Dermatitis
People typically develop this form and have symptoms in childhood. You are more like to have atopic dermatitis if your parents have it also.
Children with atopic dermatitis are more likely to develop allergies and asthma and there is a higher risk of sensitivity to foods. Some children will eventually grow out of this condition as they age.
Atopic dermatitis typically causes patches of skin that are dry and can become red, inflamed and itchy. These patches of skin will often be found on the face, neck and the creases of elbows and knees and may appear as a rash.
Scratching atopic dermatitis patches can cause fluids to ooze out and eventually may lead to thickened skin (lichenification). Areas of skin where the rash appears may also turn lighter or darker.
Causes of atopic dermatitis
The scientific explanation for atopic dermatitis is that your skin’s ability to protect you against allergens and irritants. Its natural barrier is weakened. There are a number of factors that contribute to this skin condition, such as:
- your genes
- immune system issues
- dry skin
- environmental triggers
What triggers atopic dermatitis?
There are a number of things that can trigger atopic dermatitis, including:
- exposure to allergens
- dry skin
- stress
- skin irritants, such as soaps, chemicals and even some fabrics
How to treat atopic dermatitis
There is no cure for eczema, so the goal with the treatment options is to reduce the symptoms and provide comfort.
Contact Dermatitis
If your skin shows symptoms of eczema as a reaction to substances you touch, you may have contact dermatitis. There are a couple of types of contact dermatitis; allergic contact dermatitis and irritant contact dermatitis.
Contact dermatitis may present itself with itchy bumps, fluid-filled blisters that ooze and then crust over, redness and thick or scaly skin.
Causes of contact dermatitis
Allergic Contact Dermatitis – this form is caused by a your immune system reacting to an irritant, such as latex or a metal substance.
Irritant Contact Dermatitis – this form is caused by substances, such as a chemical, coming into direct contact with your skin.
Items that may trigger contact dermatitis are:
- skin care products
- makeup
- soaps
- perfumes
- tobacco smoke
- solvents
- latex
- detergents
- nickel and other metals
Common areas eczema appears on the face
The types of eczema that are mostly like to appear on the face are:
- Contact dermatitis: This type is common in areas that are more likely to come in contact with perfumes or jewelry, such at the ears and neck.
- Atopic dermatitis: This is the most common type overall and will often appear on the cheeks, chin, around the eyes, on the eyelids and around or on the mouth
- Seborrheic dermatitis: Seborrheic dermatitis is more common around the hairline, ears, sides of the nose or even in the eyebrows.
Eczema on the lips or around the mouth
Eczema around the mouth or on the lips can look like a rash. The skin may be rough, flaky and scaly with a red, irritated appearance. When eczema occurs around the mouth or on the lips, it is referred to as lip dermatitis, or simply lip eczema. Most cases of lip eczema are atopic dermatitis or allergic contact dermatitis.
What causes lip eczema?
Just like other forms of eczema, your genes play a big part as to whether or not you’ll develop eczema. If you have lip eczema, you’ll likely experience dry, flaky skin that often peels. So, what triggers lip dermatitis? Here are some factors:
- high stress levels
- hot or cold sensitivity
- hormonal changes
- history of allergies, asthma or other forms of eczema
- skin issues or conditions that allow harmful chemicals to be more easily absorbed by the skin
- lip products, such as balms or lipstick (especially if trying them for the first time)
How do you treat lip eczema?
Treatment for eczema of this type can be difficult. To reduce the inflammation and treat lip eczema, many people use hydrocortisone cream or lip balms. These options can sometimes help, but often, the issues arise again when you stop using them. Many over the counter lip balms have no effect on your dry, flaky skin. Furthermore, some lip balms may actually worsen the problem, especially if you are allergic to any of the ingredients.
The best treatment for lip eczema is to avoid products that may irritate your skin. Often, this can be done by using ‘natural’ products that don’t contain chemicals. This is especially important for lip balms. They may seem like a quick fix for your cry, chapped lips, but they have the potential to do more harm than good when it comes to lip dermatitis. Some ingredients to avoid with lip balms are:
- fragrances
- phenol
- menthol
- vitamin E
All of these ingredients have the potential to irritate your skin, especially the sensitive skin of your lips.
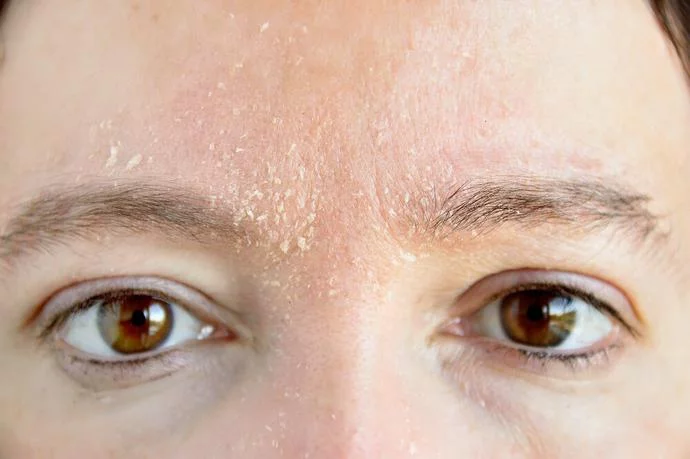
Eczema around the eyes
Eczema around the eyes is the same as eczema anywhere else on the body. People who suffer from eczema around the eyes are more susceptible to other eye problems, such as conjunctivitis, keratoconus (changes in the shape of the cornea) and an inflamed cornea. If you have eczema around your eyes and also experience eye redness, pain in your eyes, watery eyes or a sensitivity to light, you should see a doctor. Taking quick action can help eye problems from worsening. If untreated, these issues could potentially lead to loss of vision.
What causes eczema around the eyes?
Like other types of eczema, stress, allergens, environmental irritants and hormonal changes can cause flare-ups. Additionally, makeup and other cosmetics or skincare products can trigger eczema around the eyes.
How do you treat eczema around the eyes?
The sensitivity of the skin on your eyelids and face must be considered when treating these areas. For mild cases, good skincare practices may be enough. Use gentle cleansers, keep the skin hydrated, avoid hot showers (hot water may trigger eczema) and use cosmetics with moisturizing ingredients. Choose products that have hydrating ingredients like shea butter and hyaluronic acid. Stay away from ingredients that contain parabens, fragrances and retinol.
For more severe cases, non-steroidal medications are safe to use around the eyes and eyelids, because they don’t thin the skin.
Eczema on the other parts of the face
As stated previously, eczema can occur anywhere on the face. It is a persistent skin condition that is tricky to treat. Facial skin is more easily irritated and careful treatment is needed for facial eczema.
The first step is to determine which type of eczema you have. That will help determine the best treatment options, as well as give an idea of the expected outcome. Controlling eczema on the face and preventing flare-ups is usually the main objective of treatment. Although there is no cure, there are some things you can do to prevent flare-ups and treat the symptoms.
What Should Your Facial Skin Care Routine for Eczema Look Like?
To reduce the need for prescription medications and avoid flare-ups, it is recommended that your eczema skin care routine should involve the following:
- avoid scratching the affected area
- keep the skin hydrated
- avoid the use of skincare products loaded with chemicals, such as alcohol, that dry your skin out
- use moisturizers free of alcohol, fragrances or other chemicals that may irritate the skin
- bathe with lukewarm water rather than hot water
- do not over dry your skin
- avoid allergens
- try to reduce stress levels
- pat skin to dry it instead of rubbing
Other points to consider
- avoid exfoliating scrubs and toners
- consider using medical emollients to remove make-up
- for cleansing, substitute a medical emollient for soap
- if using a topical steroid, avoid the eye area
- just because a product is listed as ‘natural’ or ‘hypoallergenic’ doesn’t mean it won’t irritate your skin or cause an allergic reaction
- if you suspect that your makeup or skincare products may be an irritant, stop all and re-introduce one at a time to determine which product is causing irritation







0 Comments